What Every Phlebotomist Must Know About Drawing Coags
Drawing coags improperly has consequences
by Dennis Ernst • November 06, 2020
The multitude of ways specimen collection personnel can impact the accuracy of coagulation specimens is well documented. Patients and their physicians rely heavily on their protime and aPTT results being accurate so that the patient's anticoagulant dosage can be properly regulated. Coagulation results that are falsely lengthened or elevated can lead the physician into lowering their dose or extending the time between doses with potentially disastrous consequences. Patients who are mistakenly undermedicated can suffer strokes, myocardial infarctions, and other thrombus-related events that can be life threatening.
Alternatively, coagulation results that are falsely shortened due to specimen collection, transportation, or processing errors can mislead the physician to increase the patient’s dosage with opposite, but no less catastrophic outcomes. Coag results that are falsely shortened or lowered may prompt the physician to increase the anticoagulant’s dosage putting the patient at risk for internal hemorrhaging and the complications from blood loss.
Whether you’re a phlebotomist, nurse, physician, medical assistant, or any other professional with blood collection responsibilities, before you fill your next blue top tube, make sure you know and practice each one of these basic instructions every healthcare professional must know about drawing coags.
Ice is for colas, not coags
Putting your protimes and aPTTs on ice during transportation is so last century. It was way back in 1998 when the Clinical and Laboratory Standards Institute (CLSI) dropped the recommendation for placing coags on ice immediately after collection. That's because, when chilled, prothrombin times and INRs can be falsely shortened due to cold activation of Factor VII. Instead, transport routine coags at room temperature.
Discard the discard
Another throwback to the last century is the drawing of a discard tube to prevent tissue thromboplastin from altering coagulation results. Back in the day, it was thought that tissue thromboplastin present in human tissue could collect in the needle during insertion, enter the coag tube, and prolong the coagulation times. However, no study has ever proved it actually happened. In the late 1990s, however, many studies disproved it. Therefore, CLSI revoked the requirement for a discard tube when drawing protimes and aPTTs when the citrate tube is the first tube drawn. Even though a discard tube has not been necessary since 1998, some facilities continue to perpetuate the unnecessary practice. Studies on the necessity of a discard tube for coagulation tests other than protimes and aPTTs is circumstantial, and CLSI makes no recommendation.
Therefore, only one circumstance requires a discard tube: when using a winged collection set and the citrate tube is the first or only tube drawn. It's purpose is to remove any air in the tubing of the collection set that could cause the tube to be underfilled
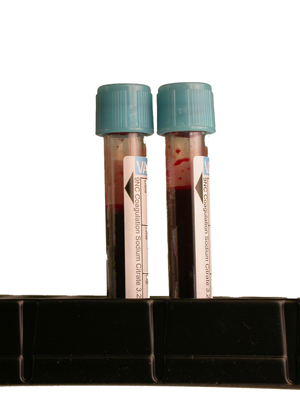
Fill, baby, fill
While it may be true that some errors affecting coagulation results run rampant in every facility, most specimen collection personnel know well that coagulation tubes cannot be underfilled and still render accurate coag results. Full tubes maintain a blood:anticoagulant ratio of 9:1. If the sodium citrate anticoagulant is in excess, as in the case of an underfilled tube, the dilutional effect of the liquid anticoagulant coupled with the excess citrate will likely yield a falsely prolonged test result. Overfilling tubes can produce falsely shortened coagulation times.
Bubble up
Every filled tube contains an air bubble. It’s this bubble that does the physical mixing of the specimen with the additive. In the case of sodium citrate (coag) tubes, the additive is a liquid anticoagulant. It mingles into the specimen with the help of the air bubble as it traverses from bottom to top every time the tube is inverted. After 3-5 inversions, the additive is fully homogenized into the specimen, and fully interrupts the clotting process. When the tube is upended, there should be a pause for the air bubble to rise to the top before uprighting it again. Simply tipping the tube from side to side with a slight jostling of the wrist does not mix the additive into the specimen. When the tube is merely jiggled back and forth, micro-clots can form, which not only wreak havoc on sensitive laboratory instrumentation, but lead to erroneous test results and the patient complications that can develop.
T-minus four hours
Once a coagulation tube is filled, significant and irreversible changes begin taking place that can alter test results. APTT results are the most susceptible to delays in testing. When testing is delayed beyond four hours, aPTT results cannot be considered valid. (If the patient is on unfractionated heparin, the citrate tube must be centrifuged within one hour of collection, and tested within four hours for reasons that will be explained later in this article.)
Prothrombin times are much more forgiving, and are stable at room or refrigerated temperatures for up to 24 hours as long as the stoppers are not removed. (Note: Stabilities vary with some testing systems.) For protimes or aPTTs, specimens that cannot be tested within the limits stated above should be centrifuged and the plasma separated and frozen for up to two weeks at -20oC. Frozen specimens should be rapidly thawed at 37oC before testing, mixed thoroughly, and tested immediately.
The one-minute rule
Everyone knows that when blood is allowed to pool below a constricted tourniquet for more than one minute, hemoconcentration begins to impact test results. Prothrombin times, fibrinogen and D-dimer are among those affected. Because coagulation proteins are large compounds, they cannot escape into the tissue below the constriction like smaller blood constituents do. Therefore, they accumulate in increasingly higher concentrations. The lack of circulation also activates platelets, which can alter coagulation factors before the specimen is even obtained.
According to CLSI, if finding and accessing a vein takes longer than one minute, release the tourniquet and allow two minutes to pass before reapplying it. This allows the blood in the affected limb to return to its basal state. Then locate and access the vein within one minute.
The Platelet Effect
Knowing how platelets work is important to minimize the potential they have to alter coagulation results during specimen processing. When platelets are removed from the body and concealed within a sodium citrate tube, they release a factor (platelet factor IV) and phospholipids into the plasma, which inhibit heparin. If the patient is taking heparin, its affect on his/her clotting abilities need to be monitored precisely. If there are too many platelets in the plasma, the patient’s heparin level will be masked, and the physician will receive a misleading result. Those who centrifuge sodium citrate tubes are responsible for making sure this doesn’t happen.
One way to prevent platelets from affecting results is to centrifuge all aPTT specimens drawn on patients receiving unfractionated heparin therapy within one hour. However, centrifugation must be of a speed and duration to render “platelet-poor plasma,” which is defined in this context as fewer than 10,000 platelets per microliter. If centrifugation is too short or of an insufficient speed, platelets will go to work falsely lowering the result and making the properly medicated patient appear undermedicated. Likewise, the over-medicated patient who needs his dosage adjusted will look perfectly medicated to the physician.

What constitutes proper centrifugation? There’s no universal speed or time that is considered standard. Every model of centrifuge has its own variables that require a calculation based on the distance from the rotor to the bottom of the tube and must take into consideration the tube manufacturer’s recommendation. Most facilities establish the centrifugation time and speed based on the equipment and tubes in use, and monitor their centrifuges’ performance regularly.
Put the pressure on
Not affecting test results, but definitely affecting the anticoagulated patient, is when insufficient pressure is applied to the puncture site. Because their blood thinner is designed to prevent clotting, bleeding after a venipuncture is much more likely. As a result, those who draw blood from patients on blood thinner must be diligent when it comes to monitoring the site prior to bandaging. Should the bandage be applied too quickly, the patient may bleed long after the collection. To make sure bleeding has stopped, remove pressure and observe the site for both superficial bleeding and hematoma formation. Taking the necessary time to assure stasis is complete can prevent the hemorrhaging of a venipuncture site, and the complications that follow.
Drawing and processing blue-stoppered tubes for coagulation studies demand a full appreciation for the affect the process can have on the test results the physician will use to medicate the patient. When healthcare professionals with specimen collection responsibilities understand and avoid the detrimental impact preanalytical errors can have on coagulation studies, they help ensure that no patient being monitored for anticoagulant therapy is medicated improperly.
Related Posts and Information
overall rating: my rating: log in to rate
blood thinner coagulation error YouTube preanalytical protime ptt
