The Order of Draw:
Do I Have To Follow It?

Yes. You do.
Evidence supporting the need for a specific order in which blood collection tubes should be filled was first published over 30 years ago, yet the concept remains elusive to many healthcare professionals with sample collection responsibilities. This article not only reinforces today’s recommended order of draw, but explains how additive carryover
during the collection process can alter the test result the laboratory reports. It also discusses what can happen when the order of draw is disregarded.
Additive carryover occurs when the needle filling a tube comes in contact with the blood/additive mixture as the tube fills, and transfers a minute amount of blood and additive into the next tube filled. This can occur with both syringe and vacuum draws. In a syringe draw, the carryover occurs with the needle of the safety transfer device. (According to OSHA, blood collected by syringe should be transferred to the tubes using a safety transfer device, not the same needle used to perform the venipuncture.) In a tube holder draw, carryover occurs from the needle within the tube holder as tubes are exchanged.
For additive carryover to occur, tubes must be filled in an inverted position so that the blood/additive mixture comes in contact with the needle that pierces the stopper. When patient positioning is such that the tubes are tilted upright relative to a horizontal plane, they fill from bottom to top. When the tube position is inverted relative to horizontal, i.e., the stopper of the tube is lower than the bottom of the tube, the tube fills from top to bottom, contaminating the needle that pierces the stopper.
In practice, those who draw blood samples cannot always control the orientation of the tubes as they are filled when using a tube holder. If all tubes could be orientated in such a manner that allowed them to be filled from bottom to top, an order of draw would not be necessary; the interior needle would never come in contact with the blood/additive mixture. However, since patients present a wide range of arm positions, and contamination of the needle that punctures the stopper cannot always be prevented, an order is necessary.
When additives carry over into a different tube type, test results may be dramatically affected. For example:
- Should the EDTA from a lavender-stopper tube, which is rich in potassium, carry over into a tube to be tested for potassium (a green-, red-, gold-, or speckle-top tube), the level of potassium may be falsely elevated leading to life-threatening medical mistakes;
- If a clot activator carries over into a tube to be tested for coagulation studies (blue stopper), the prothrombin time (PT) or activated partial thromboplastin time (aPTT) may be falsely shortened;
- When blood cultures are collected at the same time as other lab work and not filled first, bacteria from the non-sterile stoppers of the tubes can contaminate the bottles used for blood cultures.
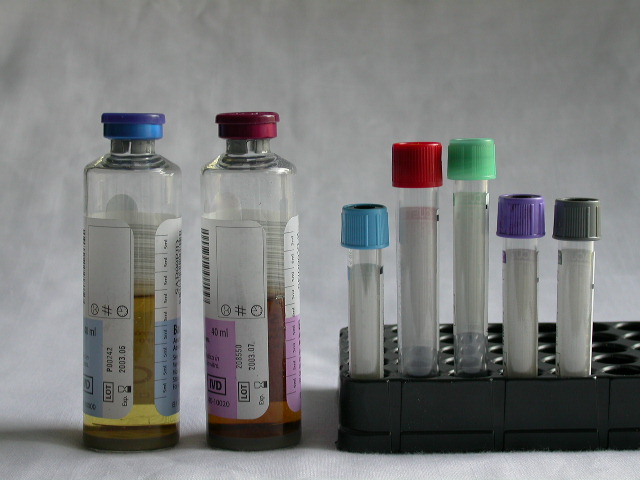
- Blood culture tubes
- Sodium citrate tubes (e.g., blue-stopper)
- Serum tubes with or without clot activator, with or without gel separator (e.g., red-, gold-, speckled-stopper)
- Heparin tubes with or without gel (e.g., green-stopper)
- EDTA tubes (e.g., lavender-stopper)
- Glycolytic inhibitor tubes (e.g., gray-stopper)
This order of draw has changed over the years, the last occurring in 2003. Necessitating the change was the industry-wide transition from glass blood collection tubes to plastic. Whereas glass is a natural clot activator, plastic is not. So in order for blood to clot in safer plastic tubes, manufacturers coat the inside of the tube with a substance to facilitate clotting, like silica particles. However, if the tube following the clot activator tube remained the coag tube, as was the recommended order prior to 2003, carryover threatens the coag results. With the consensus of all major U.S. tube manufacturers, CLSI issued one single change in the order of draw when the venipuncture standard was revised in 2003: serum tubes that used to precede the blue-stopper coag tube were relocated to follow coag tubes. This change was only possible because a myth about tissue thromboplastin was disproved.
Prior to 1998, it was thought that the trauma of a venipuncture resulted in the accumulation of tissue thromboplastin in the needle, which, if drawn into a coagulation tube, could alter results. However, because many studies have proven tissue thromboplastin not to affect PT or aPTT results when the citrate tube was the first tube drawn, it was safe for NCCLS (now CLSI) to move the serum tube immediately after the citrate tube in the order of draw.
When healthcare professionals with specimen collection responsibilities adhere to the order of draw, patients are more likely to be treated according to results that truly reflect their physiology. Neglecting this key concept can contribute to medical mistakes that can be potentially catastrophic to the patient. Because ignoring the order of draw can have severe consequences to the patient, it is critical that all who draw blood samples adhere to the established order of draw. Do you have to follow the order of draw? Absolutely.
Note: For access to any of the many articles we've written on the order of draw in our newsletter archives, simply enter "Order of Draw" in the search window at the top of this.
Additional note: For an attactive PDF of this article for posting in your facility, visit our Free Stuff page.










