Syncope Case Studies: Real Failures, Real Consequences
These are real cases. Real patients. Real verdicts.
by Shanise Keith • March 24, 2026
If you’ve read my three-part series on vasovagal syncope — the physiology, the warning signs, and the response protocol — you already know the science. You know what’s happening in your patient’s body, how to spot it early, and what to do when it progresses to a full syncopal episode. Today, I want to show you what happens when none of that knowledge is applied. What the consequences look like. What a jury decides when a phlebotomist turns their back at the wrong moment.
Case #1: Cris Nelson v. Emory Healthcare
In 2014, Cris Nelson walked into an Emory Healthcare clinic outside Atlanta, Georgia for a routine wellness exam. He was a commercial truck driver — healthy enough to hold a CDL, healthy enough to work. The blood draw was just a box to check on his way out the door.
He never drove a truck again.
The medical assistant performing the draw seated Nelson upright on an exam table. Not a venipuncture chair. Not a reclining chair with armrests. An exam table — elevated, unsupported, with nowhere for a patient to go if they lose consciousness except straight down to the floor.
During the draw, Nelson told her he felt lightheaded and dizzy. If you read Part 2 of my syncope series, you know those aren’t vague, dismissible complaints. Lightheadedness and dizziness are classic prodromal symptoms of an impending vasovagal episode. They are the body announcing, clearly and urgently, that something is about to go very wrong. The correct response is immediate: recline the patient, elevate the legs, stay close.
The MA did none of that. She turned away from the patient.
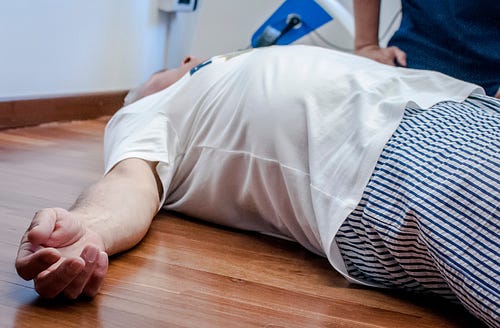
Nelson lost consciousness and fell from the table. When he regained consciousness, bleeding and laying on the floor, he told responders his arms and legs were tingling. He was transported to Atlanta Medical Center, where doctors confirmed a broken neck — a spinal cord injury at the C5-8 level. Cris Nelson was rendered a quadriplegic.
He and his wife sued Emory Healthcare, Emory Specialty Associates, and the MA for negligence and loss of consortium. Here is the detail that should stop every phlebotomist and educator cold: the defense did not contest liability. They conceded it entirely. The only remaining question was how much his shattered life was worth. A Georgia jury answered with a verdict of nearly $15 million in lifetime care costs — on top of the career that was permanently cut short at $46,000 a year.
The plaintiff’s legal argument was not complicated. It was entirely foreseeable that a blood draw could trigger syncope. Placing a patient on an exam table — without armrests, without reclining, without supervision — when that risk was known, was a failure to meet the standard of care. And when Nelson verbally signaled that something was wrong, there was still time to act. That window was not used.
Three failures. One fall. A life changed forever.
Case #2 “He Said He Didn’t Do Well With Needles”
In a case highlighted by CAP TODAY — drawn from the expert witness work of Nancy Erickson, PBT(ASCP), who has testified in more than 30 phlebotomy-related lawsuits — a young male patient told the phlebotomist directly that he did not do well with needles.
That statement alone should have changed everything. As I discussed in Part 2 of my syncope series, a patient disclosing needle anxiety or a history of problems is one of the most reliable risk flags we have. The standard response is to move that patient to a recumbent position before the draw even begins.
Instead, the phlebotomist drew him sitting up on an exam table — and then, when the draw was complete, turned her back to label the specimen.
The patient fainted. He fell to the floor and suffered brain damage and a facial injury. The case went to litigation.
What makes this case particularly instructive alongside Nelson’s is that the failure mode is slightly different. In the Nelson case, warning signs appeared during the draw and were ignored. In this case, the patient disclosed his risk status upfront, before the needle ever went in — and nothing changed. Two different points of failure. The same completely preventable outcome.
As Erickson noted, the first thing a plaintiff’s attorney will do in any phlebotomy lawsuit is subpoena the facility’s procedure manual and compare it line-by-line to the current CLSI standard. If it doesn’t reflect current guidelines — if it doesn’t address patient positioning, syncope screening, or supervision requirements — the facility has already lost the narrative. In roughly 70% of the phlebotomy cases she has reviewed, something was done against the standards.
Syncope Stats
Let’s put the phlebotomy numbers in perspective. Approximately 2.5% of patients will pass out during or immediately after a blood draw. That number climbs to 5.6% among patients who self-report a prior history of problems — which is exactly why we ask. In blood donation settings, where larger needles are used and the draw volume is higher, vasovagal reaction rates range from roughly 1% to nearly 5% depending on the study.
For diagnostic draws in hospital settings, one study of nearly 678,000 phlebotomies found a syncope rate of just 0.004% — but at that scale, even a fraction of a percent represents thousands of real patients. I think the rate of patients laying down in their beds greatly impacts this number — It’s hard to faint when laying down.
Those numbers matter because they tell us something important: syncope during needle procedures is not rare. It is an expected, predictable complication that we should be actively managing every time.
Now compare that to vaccinations. The CDC tracks post-vaccination fainting through the Vaccine Adverse Event Reporting System, and what they’ve found is striking — 7% of syncope reports after vaccination are coded as serious, and 12% of those serious cases involved head injuries. Clavicle fractures, wrist injuries, jaw fractures — all from falls. About 62% of post-vaccination syncope reports involve adolescents between 11 and 18, and roughly 80% of episodes occur within 15 minutes of the injection.
One case involved an 11-year-old girl who stood up after a flu shot, fainted, hit her face on the floor, and required hours of dental reconstructive surgery. Her family received a $39,000 settlement from the National Vaccine Injury Compensation Program — a federal program that formally recognizes vasovagal syncope as a covered injury precisely because the falls are so well documented.
My guess about why vaccination syncope rates are higher is due to the procedure being so quick. It takes a few seconds to deliver the injection. The syncopal reaction may take place a few minutes later when the patient is getting ready to leave and thinks they are fine. A blood draw takes longer, the reaction typically starts while the patient is still sitting in the chair. There is also a higher percentage of adolescents receiving their immunizations, and they are the most prone to fainting.
The procedures are different. The presence of a needle, the trigger, and the risk are not.
What These Cases Have in Common
When I look at these cases through the lens of both an educator and an expert witness, the same pattern appears every time. The risk was known. The standard existed. The standard was not followed. Someone got hurt.
In both cases, the patient was on an exam table and had their blood drawn while they were sitting up. If a patient is on an exam table they MUST be recumbent for the blood draw, even with no history of fainting.
In the first case Nelson complained of syncope symptoms during the draw, and was ignored. In the second case, a disclosed risk factor was ignored before the draw even started. In the vaccination case, the patient was allowed to stand and move too soon after the procedure. The settings are different. The injuries are different. The mechanism is identical: a foreseeable event that was allowed to become a catastrophic one.
What keeps me up at night is that none of these patients walked into a clinic expecting to be injured. They came for routine procedures. They trusted the people holding the needle. And in every one of these cases, the person holding the needle had the knowledge — or should have had the knowledge — to prevent what happened.
A Word From the Expert Witness Chair
In my years of expert witness work, I’ve seen these cases from the inside. And what I see consistently is not malice — it’s gaps. Gaps in training. Gaps between what a facility’s procedure manual says (or fails to say) and what actually happens in the room. Gaps between knowing something intellectually and being prepared to act on it under pressure.
Healthcare professionals often underestimate syncope because it’s fairly common. It’s seen as “not a big deal, it happens,” the patient recovers, everyone moves on. That familiarity breeds a kind of complacency that can be genuinely dangerous. Either that, or they have not been educated about it and have no idea how to handle it when it does happen.
The vasovagal response doesn’t care how many uneventful draws came before it. It doesn’t care that your chair “has always been fine.” It doesn’t care that the patient seemed totally okay two minutes ago.
Every time I review a case involving syncope and injury, the thought is always the same: this didn’t have to happen. Just like in the stories above, I have seen serious life-altering injuries and even deaths that occurred from falling after fainting.
Proper patient positioning, chairs with arms, laying flat on a table, reclining chairs — always use the most appropriate equipment. Screen for prior history. Never walk away from a patient post-draw. Refuse to perform a draw if a patient with syncope history won’t lay down for the procedure. These are not complex interventions. They require awareness and discipline — two things that training is supposed to provide.
If you’re an educator, ask yourself right now: do your students or employees practice the syncope protocol until it’s muscle memory? Do they know that “I don’t do well with needles” is not a throwaway comment? Do they know that their job isn’t over when the needle comes out? If the answer to any of those is no, that’s the work.
Just as Nancy Erickson stated in her case story above, when I get a new case, one of the first things I request to look at is the SOPs and training materials of the facility. If they are not aligned or up to date with CLSI they "have lost the narrative" as Nancy so eloquently put it. They will still be judged according to the standards. Most of the ones I have reviewed are woefully lacking.
The Bottom Line
Cris Nelson is a quadriplegic because a medical assistant let him sit up for a blood draw on a table, and didn’t respond when he said something was wrong. A young man suffered brain damage because a phlebotomist turned her back after completing a draw on a patient who told her upfront he had a history of problems. An 11-year-old needed reconstructive dental surgery because no one made her sit down after a flu shot.
Across all of these cases, across different procedures and different settings, the standard of care was clear. It just wasn’t followed.
The science of vasovagal syncope is not new. The standards are not new. The chairs exist. The protocols exist. The only thing standing between a routine procedure and a catastrophic outcome is the person holding the needle — and whether they’re truly prepared for the moment their patient says “I feel a little dizzy.”
Related Posts and Information
overall rating: my rating: log in to rate