Teacher Tips: Why Simulation Practice Isn't Optional
What simulation practice does for students that no lecture ever can
by Shanise Keith • April 14, 2026
Have you ever seen a phlebotomy student pick up a straight needle and hold it like a pencil?
Not a modified pencil grip, not something I could charitably interpret as an awkward-but-fixable angle. A full, fingers-curled, number-two-pencil grip on a straight needle. And they were fully prepared to insert it that way into a human arm.
They had sat through the lectures. They had watched the demo. In their mind, they understood. And then they picked up the needle and showed me something that would have made anyone scratch their head.
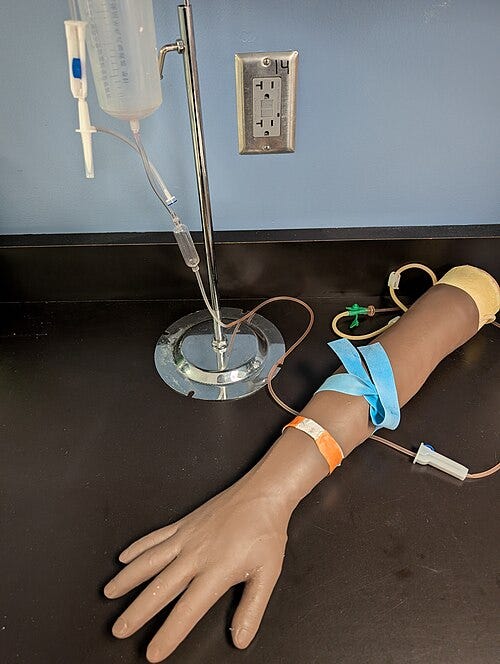
That moment — and every version of it I witnessed over the years — is why I became a passionate advocate for fake practice arms. Not as a nice-to-have, not as a budget luxury, but as a non-negotiable step in preparing students to stick real patients.
How I Was Trained (And What That Cost Us)
When I learned phlebotomy, the training model was straightforward: listen to the teacher, watch a video, watch a live demonstration, then do it yourself on a real person. That was it. That was the pipeline from novice to needle.
I didn’t think much about it at the time. That was how it was done, so I assumed that was how it should be done. When I became an instructor in the early years of my teaching career, I carried that model forward. We had a few training aids, but they weren’t a dedicated focus. Students practiced what they could, then very quickly moved to live draws.
I don’t think I was necessarily wrong to follow that model — it was what I knew, and plenty of competent phlebotomists had come out of it. But looking back now, I can see what I was missing.
When the Budget Changed, So Did the Results
As our program grew and the budget allowed, I invested in a proper set of practice arms — enough that every student could have meaningful, extended time with one before we ever moved to live practice. And with that change came a shift I didn’t fully anticipate.
The difference on that first night of live draws was not subtle.
Students who had spent a couple of hours working through the mechanics on a practice arm were noticeably more prepared. Their grip was steadier. Their angles were more consistent. They knew where the needle was going before they moved it there. They didn’t look like they were encountering the equipment for the first time, because functionally, they weren’t.
Compare that to earlier cohorts who had gone directly from seeing the equipment, listening to a lecture, watching a demo, then person to person, and the gap was clear. More hesitation. More grip adjustments mid-draw. Way more time spent with each student answering questions and fixing errors. More of that panicked pause when something didn’t feel right and they didn’t have the muscle memory to fall back on.
This wasn’t a controlled study. But I’ve been in enough clinical education to know what prepared looks like, and the arms made a measurable difference.
The Real Value: What Gets Caught Before It Reaches a Patient
Here’s the part that instructors don’t always talk about, but probably should: practice arms aren’t just for building skill. They’re for catching disasters before they happen.
And I mean that almost literally.
When students first pick up a needle in a supervised practice setting, you find out quickly what they actually understood versus what they thought they understood. Those two things are often very different.
The pencil-grip student I mentioned at the beginning wasn’t unique. Over the years I have seen students insert needles bevel-down. I saw grips and approaches I couldn’t have imagined or anticipated, because the human brain is creative in ways that instructional design simply doesn’t account for. Many times I watched students who had sat attentively through every lecture and nodded along with every demonstration pick up a needle and do something that would, on a real patient, have caused real harm.
Here’s what practice arms make possible that nothing else can: correction without consequence.
A fake arm doesn’t have nerves. It doesn’t bruise. There’s no patient sitting in the chair growing increasingly anxious while you gently explain (again) to your student that the bevel goes up. You can stop, redirect, demonstrate again, and have the student practice the correct technique immediately — on the same arm, in the same moment. The correction loop is tight. The lesson is immediate. And the patient is exactly where you want them: out of it entirely.
And to be clear — a student holding a needle incorrectly was never going to get a live stick in my program. The fake arms help students learn correct techniques, but what it really does is compress the time it takes to get past the basics. By the time my students moved to live practice, we weren’t standing there correcting grip and bevel orientation. We were working on the finer points: angle adjustment, palpation confidence, reading patient feedback, managing a difficult draw. The simulation time bought us that. It moved the floor up.
Lecture Does Not Equal Understanding
If I could go back and say one thing to myself as a new instructor, it would be this: watching is not doing, and understanding in the abstract is not the same as understanding in the hands.
Have you ever watched a skill and thought that you could easily do it, but as soon as it was your turn to perform you suddenly have no idea what the steps were? Students can absorb a lot of information in lecture format. They can follow along with a live demonstration and feel confident they’ve captured it. But the moment they pick up a needle, something changes. The knowledge has to translate into physical execution, and that translation is where things fall apart.
Motor skills don’t develop by watching. They develop by doing — and ideally, by doing with immediate feedback in a low-stakes environment. Practice arms provide exactly that. They create a space where students can fail, get corrected, and try again without any of the variables that make live practice so unforgiving.
The research backs this up clearly. A systematic review of 15 studies on clinical simulation found consistent evidence of improved student confidence in performing clinical tasks, communicating with patients, and making clinical judgments. Separate research on simulation in nursing education describes the protected environment of simulation as something that “enhances students’ self-esteem and confidence, promoting learning and substantially reducing the gap between theory and practice.” And it’s not just a short-term boost — studies have found that skill gains from simulation persist over time, with improvement documented even a month after training.
There’s also an interesting phlebotomy-specific study. Researchers who developed a simulation-based phlebotomy training program for new medical residents — people who had already completed medical school and passed board exams but had almost no hands-on draw experience — found participants rated the program between 4.3 and 4.8 out of 5 across every measure of satisfaction.
It was a short training session where they learned about venipuncture, practiced on fake arms, and then practiced on each other. Normally these medical residents learned the theory of phlebotomy in class, but were expected to perform these skills for the first time on actual patients — which is how many similar programs operate. The residents reported that it improved not only their technique, but their empathy for patients. When you’ve been on the receiving end of a needle yourself, even a simulation needle, you draw differently.
Those “pencil-grip” students? We catch it. We correct it. We have them practice the right way a dozen more times before they ever touch a real vein.
“Sink or Swim” Is Not a Teaching Philosophy
I want to address something directly, because I’ve encountered it more times than I’d like: the instructor who views practice arms as hand-holding, who believes the best way to learn phlebotomy is to simply do it on a real person and figure it out.
I understand where that mentality comes from. Many of us were trained that way. Some instructors see struggle as character-building, or interpret structured simulation as coddling students who need to toughen up. And there’s a kernel of truth buried in there somewhere — students do eventually need to work through the discomfort of live practice, and over-sheltering them creates its own problems.
But there is a meaningful difference between productive discomfort and avoidable harm. Sending an unprepared student to practice on a real person isn’t grit-building. It’s a failure of scaffolding.
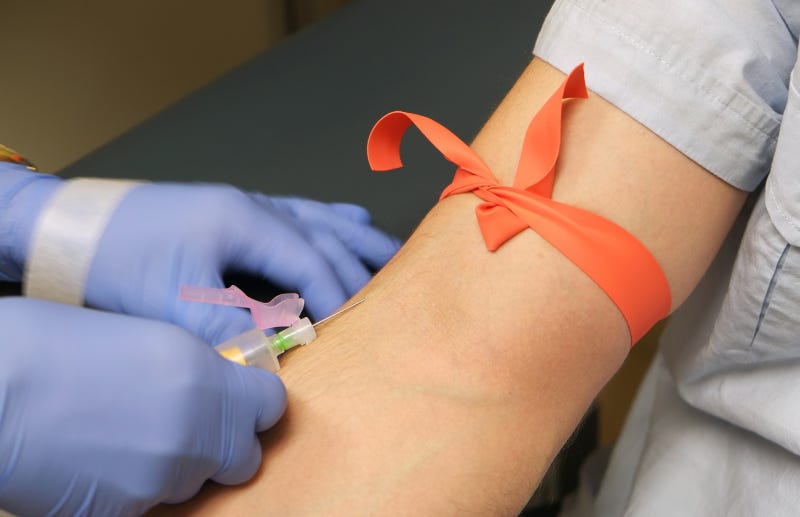
Think about what it actually feels like to perform a clinical skill on a live human being for the very first time, with no prior hands-on preparation. The anxiety is real. The physical feedback is different from anything you’ve encountered on a model or in a video. The patient is watching you. Your hands may be shaking. That is not the moment to also be figuring out how to hold the needle, or how to activate the safety.
I’ve been that student. The first time I drew blood was on a real person, with a demonstration and nothing more behind me. I got through it, but I was terrified — and I was operating on adrenaline more than skill. When I think about my situation I wish I had the opportunity to spend more time practicing and understanding, rather than just trying to mimic what I had watched.
Our job as instructors isn’t to see who survives. It’s to prepare students so thoroughly that their first live draw feels like the next logical step in a progression — not a leap off a cliff.
A Note for Programs With Limited Budgets
I know not every program can afford a full classroom set of training arms, because I was running one of those programs once. If your budget is limited, here’s what I’d say: even one or two arms, used strategically with small groups or as a rotation station, is better than none. Students benefit from even an abbreviated session if it’s structured and supervised.
There are several versions available out there that are extremely affordable compared to how much they cost ten years ago ($500+). They start around fifty dollars on Amazon. It’s worth it to have a few.
The goal isn’t perfection before live practice. It’s baseline competency, verified technique, and at least some opportunity to fail safely before the stakes go up.
Future patients will thank you for it, even if they never know the planning and practice that a student goes through to be properly trained.
Related Posts and Information
overall rating: my rating: log in to rate
simulation lab Center for Phlebotomy Education gifts for phlebotomists lab week Phlebotomy